
If you face Psoriasis, You how devastating this disease is…
Very often you just desperately trying to find the ”super treatment” but without any success…
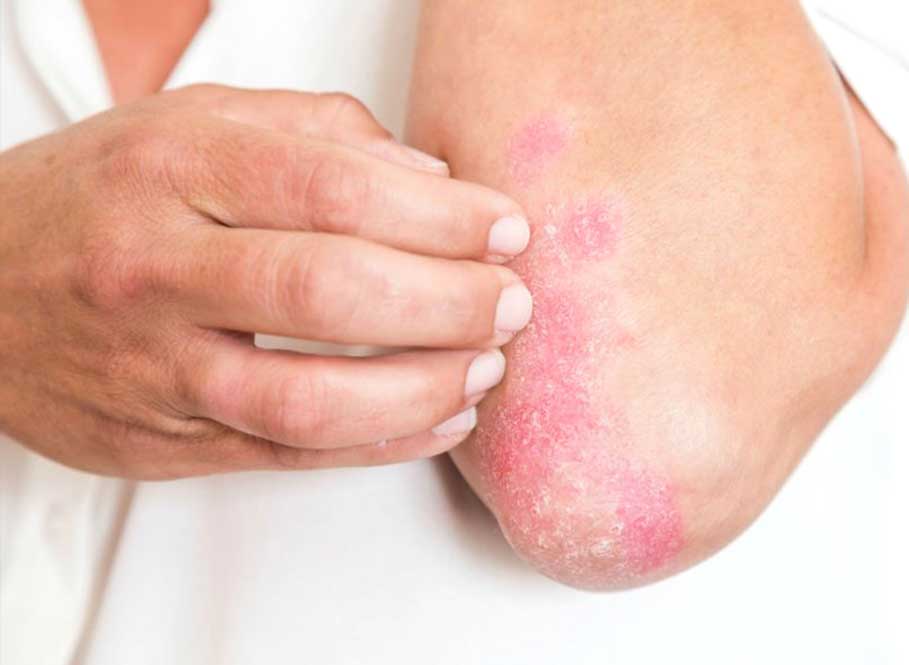
According to psoriasis.org — Psoriasis typically affects the outside of the elbows, knees or scalp, though it can appear on any location.
Some people report that psoriasis is itchy, burns, and stings.
Psoriasis is associated with other serious health conditions, such as diabetes, heart disease, and depression.
Psoriasis is a chronic disease — it means that it lasts 1 year or more and require ongoing medical attention or limit activities of daily living or both.
It is benign and not contagious? The cause of psoriasis is unknown. It is not contagious but often occurs in certain families. The disease typically appears for the first time in young adulthood with red, thickened skin areas covered with white scales. Commonly, the knees and elbows are affected, but psoriasis can appear anywhere on the skin.
Celebrities Raising Awareness for Psoriasis
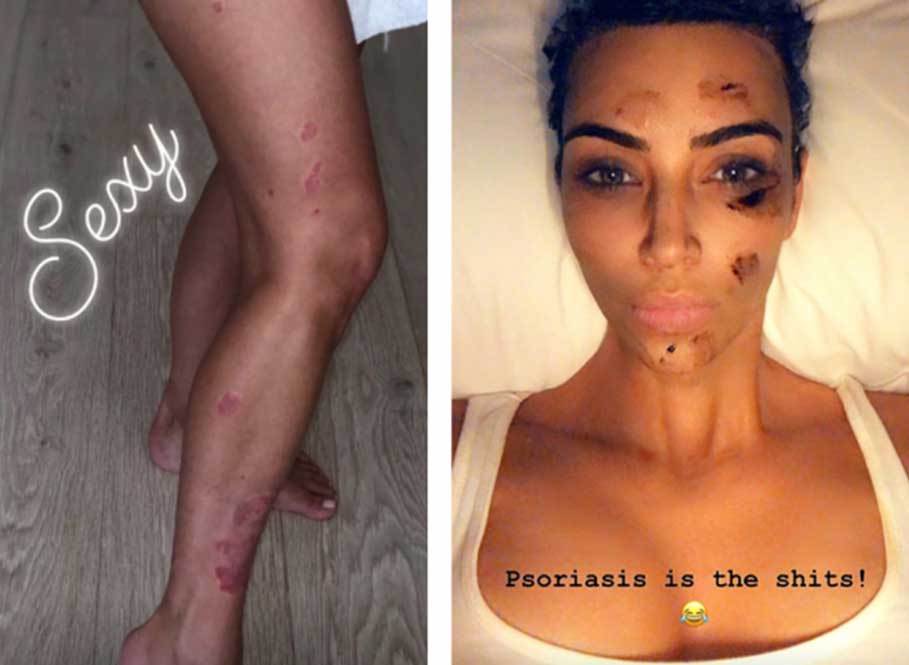
Kim Kardashian’s Psoriasis Journey
Kim Kardashian, one of the most famous faces in pop culture, has publicly shared her struggles with psoriasis for years. Her openness about the condition has made her a key advocate for raising awareness. Kim has frequently discussed her flare-ups and the impact it has on her life, particularly given her position in the spotlight.
Cara Delevingne’s Struggles and Advocacy

Supermodel Cara Delevingne has spoken about her battle with psoriasis, particularly during the height of her modeling career. Stress, which is a known trigger for the condition, often exacerbated her symptoms during fashion shows. Cara’s decision to speak out about her experience has helped normalize psoriasis in the beauty industry, where appearances are heavily scrutinized.
LeAnn Rimes’ Experience
Country singer LeAnn Rimes has been very open about her lifelong battle with psoriasis, which began when she was just two years old. Over the years, she has shared her experiences and treatments, and her advocacy for the condition has helped many feel less alone in their journey.
Treatment Options Celebrities Use
Topical Treatments Celebrities Swear By
Many celebrities, like Kim Kardashian, use topical treatments such as corticosteroids, vitamin D analogs, and salicylic acid to manage flare-ups. These treatments are applied directly to the skin to reduce inflammation, scaling, and itching, and they remain a cornerstone of psoriasis management.
Phototherapy and Its Popularity Among Celebrities
Phototherapy, also known as light therapy, has been a go-to treatment for several celebrities dealing with psoriasis. This treatment involves exposing the skin to ultraviolet light under medical supervision, which slows down skin cell turnover. Kim Kardashian and LeAnn Rimes have both spoken about the benefits of phototherapy in their treatment regimens.
Systemic Medications: Injections and Pills
For more severe cases of psoriasis, celebrities like Cara Delevingne have turned to systemic treatments, which include injections or pills that work throughout the body to reduce inflammation. Biologics, a type of medication that targets specific parts of the immune system, have become a popular option for those with moderate to severe psoriasis.
Alternative and Holistic Approaches Celebrities Try
Celebrities are also known to explore holistic and alternative treatments for psoriasis. From diet changes to acupuncture and herbal remedies, stars like LeAnn Rimes have embraced these methods alongside traditional medical treatments. Natural remedies like aloe vera, turmeric, and fish oil are often cited as beneficial for reducing inflammation.
Kim Kardashian’s Approach to Psoriasis
Kim’s Diet and Lifestyle Changes
Kim Kardashian has been vocal about making diet and lifestyle changes to manage her psoriasis. She has experimented with cutting out foods like gluten and dairy, which are believed by some to trigger inflammation. Kim also practices stress-reduction techniques, such as meditation and exercise, which can help keep flare-ups at bay.
Skincare Routines Kim Uses for Psoriasis
Kim Kardashian has shared details about her skincare routine, which includes moisturizing creams and oils to keep her skin hydrated and soothe irritated patches. She often uses products containing ingredients like hyaluronic acid and ceramides to help restore the skin’s barrier and prevent dryness.
Medical Treatments Kim Has Explored
In addition to topical creams and light therapy, Kim has tried more advanced medical treatments, such as biologic injections. These treatments help target the underlying immune response that causes psoriasis, offering long-term relief for many patients.
Cara Delevingne’s Fight Against Psoriasis
The Role of Stress in Cara’s Psoriasis
Cara Delevingne has been candid about how stress plays a significant role in her psoriasis flare-ups. During high-stress events, such as fashion week, her psoriasis would worsen, affecting her confidence on the runway. To combat this, Cara has turned to relaxation techniques, such as yoga and mindfulness, to help manage her stress levels.
Cara’s Embrace of Body Positivity Despite Psoriasis
Despite the challenges psoriasis poses, Cara has embraced body positivity and continues to work as a model, even during flare-ups. By sharing unfiltered images of her skin, Cara has become an advocate for self-acceptance, encouraging others to embrace their natural beauty.
How Cara Incorporates Fashion and Makeup to Conceal Flare-Ups
Cara has also developed creative ways to conceal her psoriasis during public appearances. She uses long-sleeved clothing, high-necklines, and makeup techniques to hide flare-ups while maintaining her signature style on the red carpet.
7. LeAnn Rimes’ Holistic Psoriasis Management
LeAnn’s Advocacy for Open Conversations About Psoriasis
LeAnn Rimes has been an outspoken advocate for open and honest conversations about psoriasis. She has shared her personal experiences in interviews and on social media, encouraging others to speak up and seek help for their condition.
The Healing Power of Music and Psoriasis
Music has played a therapeutic role in LeAnn Rimes’ psoriasis management. She has often spoken about how singing and songwriting help her cope with the emotional strain of living with a chronic illness. For LeAnn, music provides both an emotional outlet and a form of relaxation.
Natural Remedies LeAnn Incorporates
In addition to traditional medical treatments, LeAnn Rimes incorporates natural remedies into her psoriasis care routine. She uses ingredients like coconut oil and essential oils to soothe her skin, along with adopting a diet rich in anti-inflammatory foods.
Insights from Dermatologists and Experts
Expert Opinions on Celebrity Treatments
Dermatologists often highlight that while celebrity treatments can be effective, it’s essential for patients to consult with a healthcare provider to create a treatment plan tailored to their specific needs. Celebrities like Kim Kardashian may have access to advanced therapies, but many of these treatments are available to the general public as well.
Case Studies of Effective Psoriasis Treatments
Several case studies have shown the effectiveness of treatments like biologics, phototherapy, and lifestyle changes in managing psoriasis. These studies confirm that with the right combination of therapies, patients can achieve long-term remission.
The Future of Psoriasis Treatment
Emerging Treatments and Research
The future of psoriasis treatment looks promising, with ongoing research into new medications and therapies. From biologics that target specific immune cells to gene therapy, advancements in treatment are helping patients achieve clearer skin with fewer side effects.
Psoriasis in the Era of Personalized Medicine
Personalized medicine is becoming a game-changer in psoriasis care. Treatments can now be tailored to an individual’s unique genetic makeup and immune response, allowing for more effective management of the disease.
The Role of Technology in Managing Psoriasis
Technology is also playing an increasing role in psoriasis management. Apps that track flare-ups, virtual consultations with dermatologists, and wearable devices that monitor skin health are becoming valuable tools for patients.
Practical Tips for Managing Psoriasis
Tips Inspired by Celebrity Routines
Drawing inspiration from celebrities like Kim Kardashian and LeAnn Rimes, patients can implement several lifestyle changes, such as adopting a skin-friendly diet, practicing stress management techniques, and establishing a consistent skincare routine.
How to Stay Positive During Psoriasis Flare-Ups
Staying positive during flare-ups can be challenging, but building a strong support system and practicing self-care can make a significant difference. Celebrities often share their struggles publicly, reminding others that they are not alone in their journey.
Building a Support System for Psoriasis Management
Support from family, friends, and healthcare professionals is crucial in managing psoriasis. Celebrities like Cara Delevingne have shown the power of surrounding yourself with positive influences, whether through therapy, support groups, or close relationships.
11. Conclusion
Key Takeaways on Celebrity Psoriasis Management
Celebrities like Kim Kardashian, Cara Delevingne, and LeAnn Rimes have helped bring psoriasis into the public eye, showing that it is a manageable condition with the right treatments and support. Their openness has empowered others to seek help and explore various treatment options.
Encouraging Awareness and Empathy
By sharing their personal journeys, these celebrities have played a pivotal role in raising awareness for psoriasis. Their stories encourage empathy, reduce stigma, and inspire others to embrace their unique skin, reminding us all that even the most famous faces can face similar struggles.
Sometimes you can be misled:
If you’re experiencing uncomfortable patches, scales, or redness on your skin, you may be wondering if you have psoriasis or rosacea. (About rosacea you can read in this article: What Triggers Rosacea? How To Fight Symptoms and Treat This Disease.
Even most famous people like Kim Kardashian West can’t rid of psoriasis. Her quote about this disease:
If you have psoriasis, you can’t let it ruin your life or get the best of you. @KimKardashian
Cara Delevingne, an in-demand model says that she has this disease. Here are some quotes from her:
- ”Just to reiterate, I have psoriasis and it’s leaves scares and I will have for the rest of my life [sic]”
- ”I can handle the negative comments but just remember that no one is perfect.”
- ”EMBRACE YOUR INDIVIDUALITY! It makes you who you are x.”
It only happened during the Fashion Weeks, which are, of course, the worst time of year for me to be covered in scabs. Psoriasis is an auto-immune disease, and I’m sensitive. @Cara Delevigne.
What Are The Most Common Causes of Psoriasis?
In psoriasis skin, the cells of the epidermis divide approximately 7 times faster than normal.
Although Psoriasis has nothing to do with cancer, according to Harvard Medical School it still can cause some types of cancer:
The researchers found that people with psoriasis had an increased risk of developing cancers including colon, kidney, laryngeal, liver, lymphoma, non-Hodgkin lymphoma, esophageal, oral, and pancreatic cancers.
Worth reading: How to Reduce Your Risk of Breast Cancer. [Info Graphic]
They also found that people with severe psoriasis who developed cancer also had an increased overall risk of dying.
The rapid cell division is accompanied by decreased cell maturation.
This entails a heavy scale formation.
The rapid cell division and insufficient cell maturation are caused by signal substances released from white blood cells (lymphocytes).
You might be interested: Health Benefits Of Dandelion Flower: Heals The Skin, Helps To Lose Weight, Protects Against Cancer
The activation of lymphocytes is probably essential for the development of psoriasis.
What Worsens Psoriasis? The Most Common Aggravating Factors.
Psoriasis can occur on areas of skin that are damaged by scratching, rubbing, or severe sunburns.
Similarly, certain infections, particularly streptococcal throat infection, can cause a new outbreak or aggravate an existing outbreak.
Stress and alcohol consumption are also common aggravating factors.
You might like: Gestational Diabetes? The Best Way To Deal With Pregnancy Risks.
Certain medications such as lithium, beta-blockers and anti-malarial drugs can sometimes induce an aggravation.
The disease is also influenced by climate.
It is common for the disease to worsen during winter and improve during summer.

Different types of Joint and Nail Psoriasis.
Psoriasis appears in a variety of forms.
Nails and joints can be attacked.
The most common form appears with red, thickened areas that are covered with thick, white scales.
Related: Raspberry Oil Features: New Super Way Of Skin Moisture And Elasticity
These areas are well-demarcated in relation to the normal skin, but the affected areas can flow together.
All skin areas can be attacked, but many patients experience the affection of knees and elbows.
It is common for both the right and left sides to be attacked at the same time.
The disease is also commonly appearing in the scalp area causing annoying dandruff formation.
For some, especially overweight patients, the disease can occur in the skin folds.
The heavy scale formation is rarely seen in the skin folds.
Nail Psoriasis
When the nails are attacked, it manifests itself with small indentations in the nail plate (called ‘pittings’) or partial loosening of the nail.
This loosening causes a yellow discoloration.
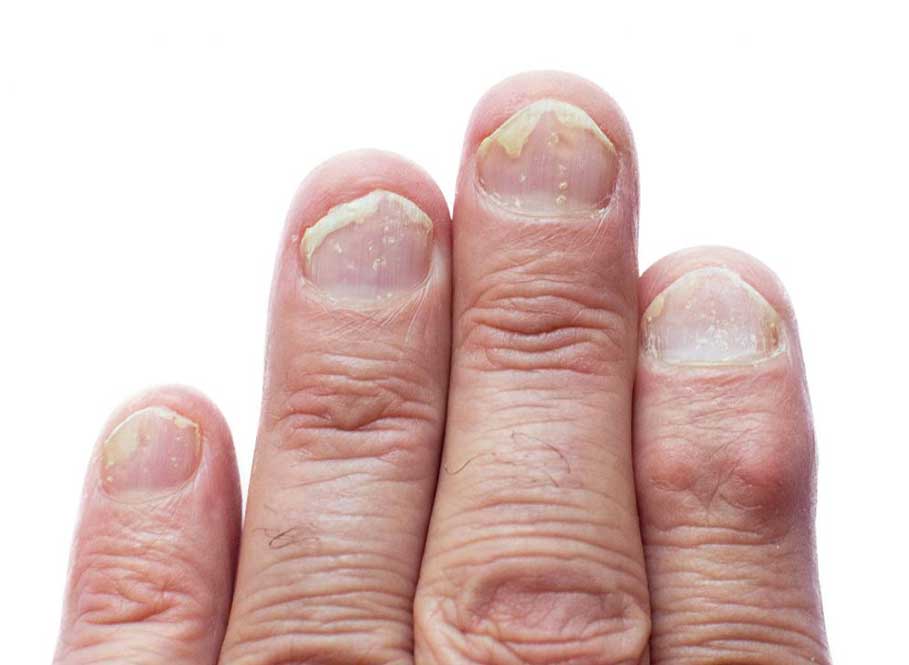
In the most severe cases, the nail plate thickens or crumbles.
Approximately 50% of patients with psoriasis have some nail involvement, and the lifetime incidence of nail disease is estimated at 80% to 90%.
Nail disease may rarely be the only manifestation of psoriasis.
More important, nail psoriasis can cause significant pain and discomfort, leading to impairment in quality of life and work function.
You might like: Discover the Power of Postbiotic Skincare
There is a strong correlation of nail psoriasis with psoriatic arthritis.
Patients with psoriatic arthritis have rates of nail disease as high as 70%.
There is evidence that nail psoriasis may be a predictor of the joint disease developing later in life.
Fingernail psoriasis is more problematic for many patients than toenail disease.
In addition, psoriatic toenails are often secondarily infected with dermatophytes, which may complicate treatment assessment.
Treatment with immunosuppressive medications may even contribute to the development of onychomycosis in patients with toenail psoriasis.
For these reasons, most studies evaluate fingernail psoriasis alone.
Nail Psoriasis Treatment
An array of treatment options are available for nail psoriasis, including topical products, procedural interventions, and oral-systemic and biologic agents.
The challenges of treating nail disease are poor penetration of topical therapy into the nail and surrounding tissue, pain associated with intralesional injections, adverse effects, and monitoring of systemic therapies and patient adherence to therapy.
Check this article: Fat Is Good! Best Oils For Women’s Skin, Hair, and Body.
Because many of the treatments most commonly used to treat psoriasis do not have published, randomized, double-blind, placebo-controlled trials addressing nail disease, the recent Cochrane review does not help dermatologists make an informed decision regarding the best treatment for a patient with nail psoriasis.
Nail Psoriasis Treatment Recommendations:
Treatment recommendations for 4 clinical nail psoriasis scenarios were developed based on the evidence reviewed in the study and expert opinion from the Medical Board of the National Psoriasis Foundation.
- Patients with psoriasis limited to the nails. These patients have minimal or no skin disease and no evidence of joint disease, with 3 of 10 fingernails having onycholysis, pitting, and distal hyperkeratosis. These patients are embarrassed by the appearance of the nails and have mild pain with use. No previous therapy has been used. High-potency topical corticosteroids alone or in combination with calcipotriol were recommended with enthusiasm, and intralesional corticosteroids were recommended. Systemic and biologic treatments were not recommended for this patient scenario.
- Patients with psoriasis limited to the nails for whom topical therapy has failed. These patients have 5 of 10 nails involved and moderate to severe nail pain. The medical board recommended the following in ranking order from highest enthusiasm to lowest: adalimumab, etanercept, intralesional corticosteroids, ustekinumab, methotrexate, and acitretin.
- Patients with psoriasis of the skin and nails. These patients have psoriasis on 8% of their body surface area, 5 of 10 nails with severenaildystrophy,andmoderate to several associatedpain. Topical therapies have proven inadequate to control the disease. The board recommended adalimumab, etanercept, and ustekinumab with high enthusiasm; methotrexate, acitretin, infliximab, and apremilast were also recommended.
- Patients with skin, joint, and nail disease. These patients have skin disease on 8% of their body surface area, a history of dactylitis and morning stiffness (psoriatic arthritis), and 5 of 10 nails with severe nail involvement and pain. The recommendations for treatment were, in ranked order from the highest to lowest: adalimumab, etanercept, ustekinumab, infliximab, methotrexate, apremilast, and golimumab.
Rare Forms of Psoriasis
Especially with young people, a certain form of psoriasis can occur following a throat infection.
This form appears with large drop-shaped, red bumps that can attack large areas of the skin.
It is common for such acute outbreaks to disappear after a few weeks.
In addition to these common forms of psoriasis, rare pustular psoriasis also exists.
It is characterized by red skin areas dotted with yellow pus-filled blisters.
Related: Pamper Yourself: Homemade Beauty Treatments. Cheap Face Masks.
This form of psoriasis is not contagious either.
Psoriatic Arthritis. Facts and Treatment.
About 20% of patients with psoriasis suffer from a special form of psoriatic arthritis.
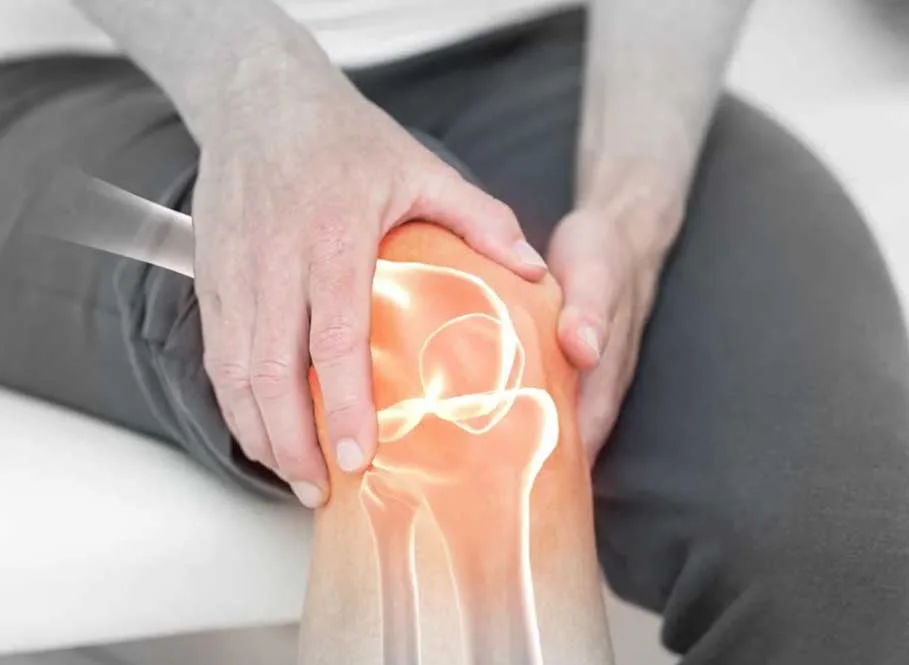
Psoriatic arthritis can usually be diagnosed by examining its distribution in the joints and on the x-rays changes.
Psoriatic arthritis is a chronic inflammatory skeletal disease associated with health concerns such as obesity, type II diabetes, dyslipidemia, hypertension, and cardiovascular disease.
The role of these metabolic factors in the pathogenesis, severity, and progression of psoriatic arthritis remains unclear.
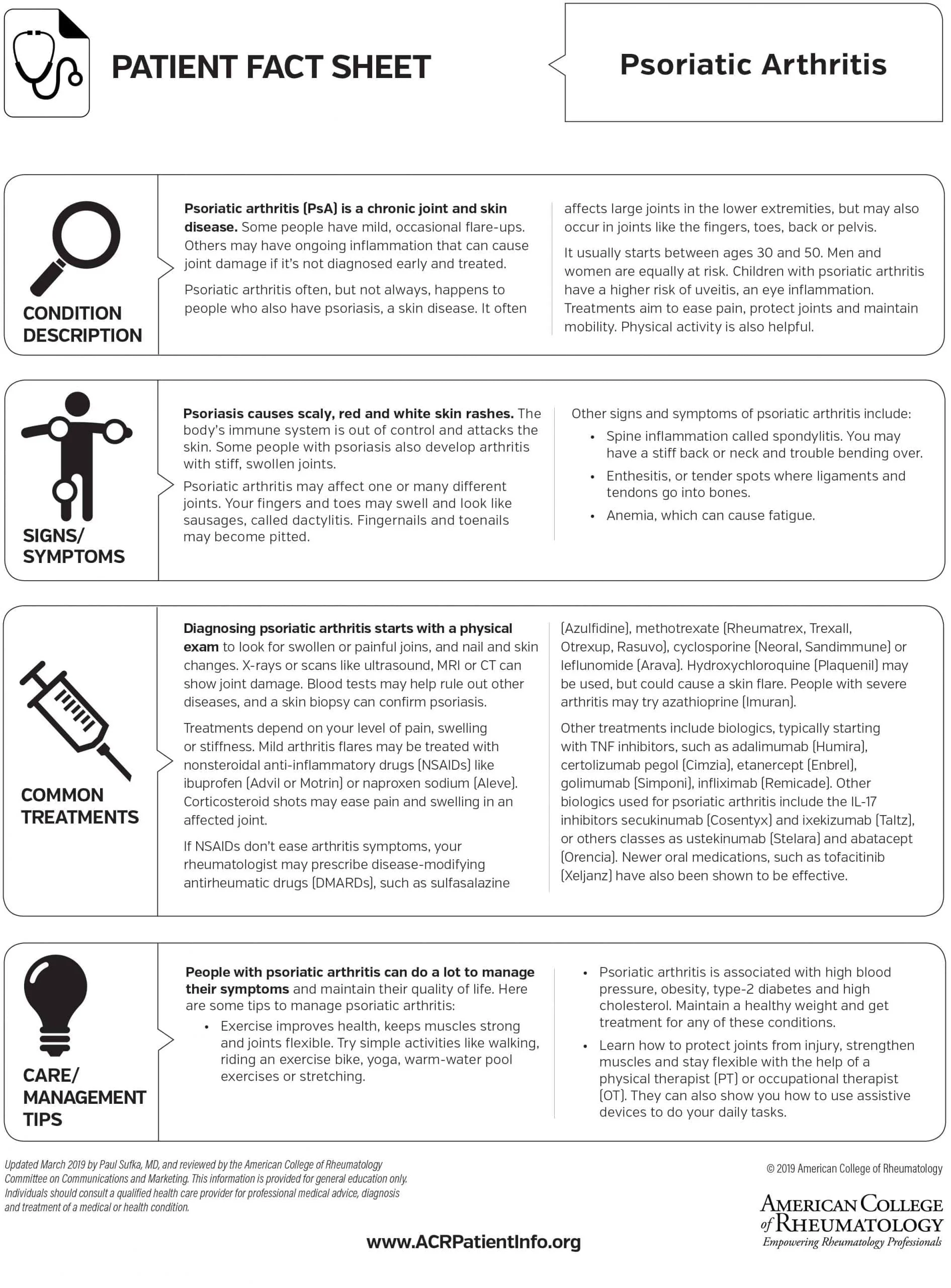

Diagnosing Psoriatic Arthritis
Early psoriasis recognition, diagnosis, and treatment of psoriatic arthritis can help prevent or limit the extensive joint damage that occurs in later stages of the disease.
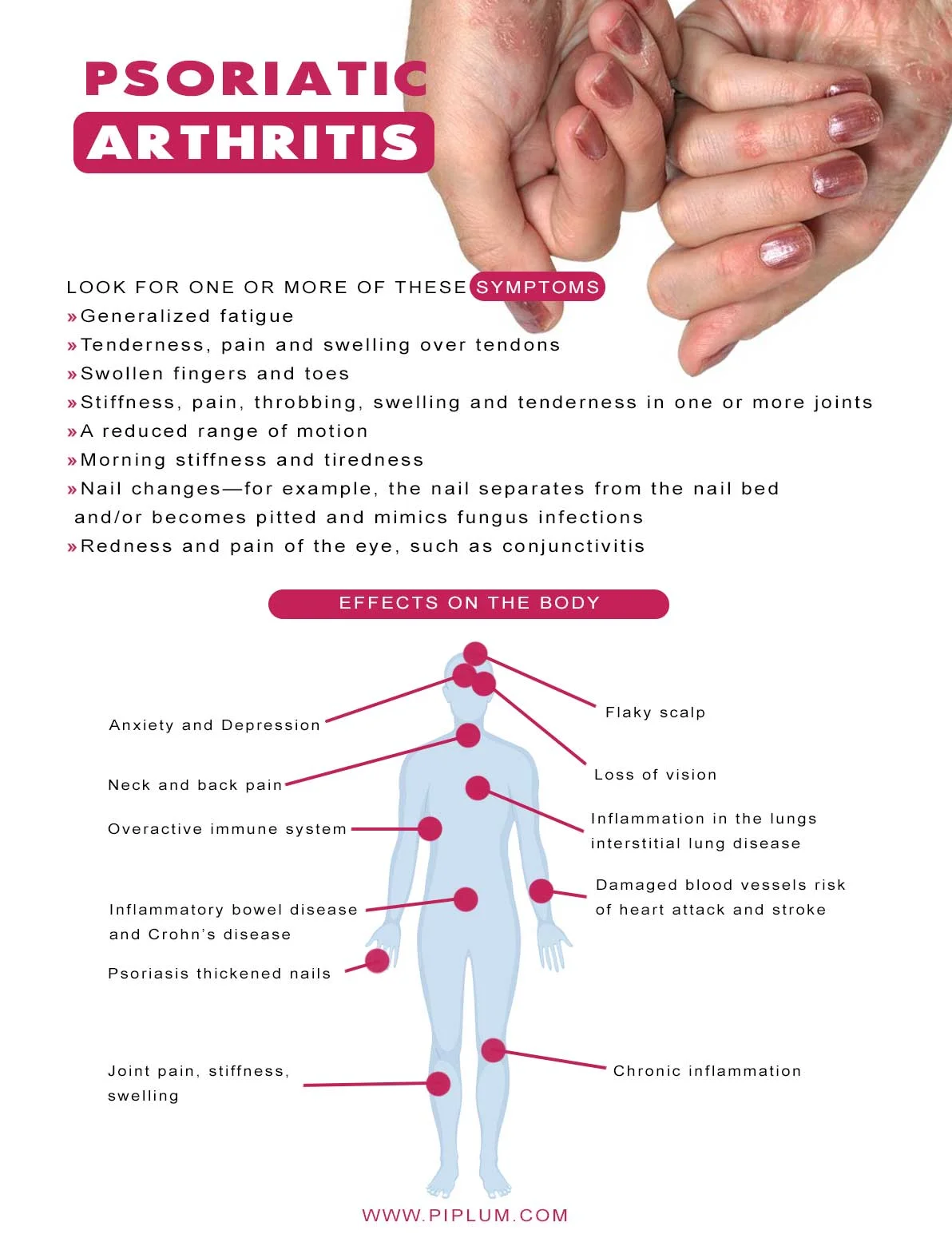
How is Psoriasis diagnosed?
A doctor can usually diagnose psoriasis by examining the skin.
In case of doubt, a skin sample is taken which is then examined under a microscope.
The diagnosis cannot be made based on a blood sample.
How is Psoriasis Disease Treated? Treatment Drugs and Tips.
Psoriasis cannot be cured. But there are some effective remedies to reduce symptoms.
Here are tips on how to treat Psoriasis. Treatment methods by Celebrities:
- Sun exposure
- Baths
- Probiotics
- Occlusive dressings
- Topical preparations for psoriasis
- Emollients
- Topical steroids
- Vitamin D-like compounds
- Tar
- Dithranol
- Calcineurin inhibitors
- Tazarotene
- Ultraviolet treatment for psoriasis
- Narrow ultraviolet B
- Psoralen and ultraviolet A
- Systemic non-biological medication for psoriasis
- Methotrexate
- Ciclosporin
- Acitretin
- Apremilast
- Fumaric acid esters
- Other non-biological medications
- Biological therapies
Topical treatment, systemic treatment (tablet or injections) and phototherapy can be used to keep psoriasis at rest.
Since the disease has many different degrees of severity, the treatment of psoriasis is carried out according to the individual patient’s needs.
In addition, the disease sometimes varies to such an extent that each individual patient may need to be given different treatments at different times.
There is no treatment able to cure the disease. Don’t be hooked on the fake ads!
The purpose of the treatment is, therefore, to make current outbreaks disappear.
A distinction is made between topical treatment, phototherapy, tablet treatment, and biological treatment.
In addition, these treatments can be given in different combinations.
In most cases, the treatment is carried out at home, while there is rarely a need for hospitalization.
Steroids (adrenocortical hormone preparations)
Steroids come in various strengths both as an ointment, cream, gel, and solution.
The strong preparations have a rapid effect; but they also have side effects including thin skin, enlarged blood vessels and the tendency of superficial skin hematomas after prolonged use.
By following the doctor’s treatment instructions, side effects can most often be avoided. The side effects are most often visible in the face and on skin folds.
Be aware that sudden cessation, especially with the strong preparations, may cause a transient aggravation of the disease.
Combination of vitamin D and steroids
An ointment containing both a steroid and calcipotriol (Daivobet®) is more effective than each drug alone.
Treatment with this kind of combination is suitable for many patients.
Coal Tar For Skin Treatment
Tar is one of the oldest known preparations used for treating psoriasis.
Topical application of coal tar has been used to treat skin diseases for more than 2000 years is an effective therapy for reducing skin inflammation and itch while improving the skin barrier function.

Tar smells and discolors, and it can increase the skin’s sensitivity to sunlight, but the tar treatment is without major side effects.
It is a well-known fact that tar in certain contexts can be carcinogenic, but numerous studies have shown that tar treatment of psoriasis patients do not result in an increased risk of developing skin cancer.
Tar can be used in both ointments and pastes, but pure tar can also be smeared on the skin.
This treatment can be combined with a hot shower.
Tar baths are especially used during hospitalization at a dermatology department.
Phototherapy. Sunlight For Psoriasis Treatment.
Different types of ultraviolet light, sometimes in combination with tablets (PUVA), can improve psoriasis.
The ultraviolet rays in sunlight can improve psoriasis symptoms.
Dr. Julie Moore of Gottlieb Memorial Hospital says that sunlight is one of the best ways to treat psoriasis, so she recommends that her patients “sit out on the deck and give their affected areas a good sunbath.

The same ultraviolet rays can be formed in fluorescent tubes of different types.
Some tubes produce ultraviolet light of type B (UVB).
This kind of ultraviolet light improves psoriasis after approx. 30 treatments given 2-3 times weekly.
During the treatment period, the amount of light is gradually increased in order to accustom the skin to the ultraviolet rays.
UVB treatment can be given by practicing dermatologists and dermatology departments.
PUVA is another kind of phototherapy.
P stands for psoralen which is a substance that increases the skin’s sensitivity to ultraviolet light.
UVA stands for ultraviolet light of type A.
When receiving PUVA treatment, the patient should take psoralen tablets prior to UVA irradiation.
Psoralen accumulates in the lens of the eye.
In order to avoid eye side effects, sunglasses must be worn when staying outdoors in the sunshine on the day of treatment.
Tanning solariums emit almost pure UVA radiation.
So, if you are using solariums for psoriasis treatment, you need to be aware of that there is no such thing as a safe tan from a solarium.
It is a myth that using a solarium is a safe way to tan and protect your skin from burning in the sun.
Solarium tans offer no protection against DNA damage to skin cells, which can occur without any visible signs of skin damage.
The effect of solarium treatment on psoriasis is limited.
Prolonged, intense exposure to ultraviolet light can increase the risk of premature aging of the skin and the development of skin cancer.
With the knowledge we have today, it seems, however, that the use of ultraviolet light as a treatment only increases the risk of skin cancer on a very low level.
The types of skin cancer that can occur are slow-growing and can be cured.
Tablet treatment for Psoriasis
Tablet treatment with methotrexate, acitretin (Neotigason®) or ciclosporin (Sandimmun®) is used to treat severe psoriasis.
Tablet treatment is used in rare cases and only for psoriasis patients for whom other treatments have not had an effect.
Acitretin is related to vitamin A.
More about vitamin-rich food read here: Do You Really Know The Truth About the Food You Eat? [11 Myths]
Acitretin can result in a significant improvement, but this improvement is often accompanied with side effects, especially in terms of dryness and flaking of the mucous membranes; just as there can be seen an impact on the liver function and an increase of the content of certain fats in the blood.
It is therefore important to arrange regular consultations with the doctor during an acitretin treatment.
Acitretin is teratogenetic and is slowly excreted from the organism.
It is thus important that women are protected against pregnancy during and following treatment.
Methotrexate is a so-called cell poison.
With psoriasis, methotrexate is given in such small quantities that only the immune system is affected.
How to strengthen the immune system read here: Discover Immune and Nervous System Strengthening oil – Flaxseed Oil
Methotrexate is one of the most effective means for the treatment of psoriasis.
When initiating a methotrexate treatment, blood samples must be taken once a week.
Later on, monthly blood samples will be sufficient.
Ciclosporin affects the immune system of the organism, and it, therefore, has a very good effect on even severe psoriasis outbreaks.
However, treatment with ciclosporin can increase blood pressure and decrease renal function.
Therefore, ciclosporin is not suitable for long-term treatment.
Psoriasis Biological treatment
Biological drugs are proteins, usually antibodies, specifically designed to affect the activation of the immune system in the skin.
Compared to traditional treatment, biological therapy can have similar or even fewer side effects.
The treatment is expensive.
So far these drugs are approved for treatment of severe psoriasis which cannot be satisfactorily treated in any other way:
The biological substances are given as an injection either in a vein (at the hospital) or beneath the skin (by the patient him/herself).
Climate therapy
Climate therapy can sometimes be chosen over hospitalization.
Climate therapy lasts 4 weeks and is commonly carried out at the Dead Sea in Israel.

The most important part of the treatment is the sunbeams which especially in this geographic area contain many UVA rays.
In addition, the patients bathe in the Dead Sea which has a very high salt content.
Climate therapy often results in total improvement of the skin; however, as with the other treatments, psoriasis will reappear at one time or another.
Some places like Blue Lagoon in Iceland tells that the efficacy of Blue Lagoon geothermal seawater for treating psoriasis has been confirmed through decades of research.

Experimental treatment. Leech therapy for Psoriasis.
Extensive research is being conducted in the field of psoriasis, and new treatments are being tested.
However, the road from the first testing of a new product to its availability at the pharmacy is long.

These are a few of the clinical success stories with leeching.
Its effect on venous congestion packed with its biomolecules is definite to show more wonderful effects on other dermatological problems as well.
Skin disorders primarily of an autoimmune kind make the dermis thick with poor tissue perfusion.
The leech saliva prevents inflammatory mediators, decreases tissue thickness, accelerates reperfusion, and increases the permeability of the tissue making it more acceptable to therapeutics. Hence making leech therapy an ideal mode of treatment in
dermatology.
Leech is a boon to dermatologists but its use must be with caution as it’s known to have its own type of side effects.
You might like: The truth is that the more you learn about buckwheat, the more you want to eat it every day.







